A dental abscess is more than severe tooth pain—it’s a dangerous tooth infection that can spread quickly if left untreated. For adults in and around Lansing, knowing when tooth pain becomes a true emergency can prevent a simple infection from turning into a hospital visit.
Many people hesitate to call a dentist right away, hoping the pain will fade. Unfortunately, dental abscesses do not heal on their own, and delays can increase both health risks and treatment complexity.
Quick Answer: Is a Dental Abscess an Emergency?
Yes. A dental abscess is always considered an emergency.
Even if pain temporarily improves, the infection remains and can become life-threatening if untreated. Before Dentistry, dental infections were a leading cause in death.
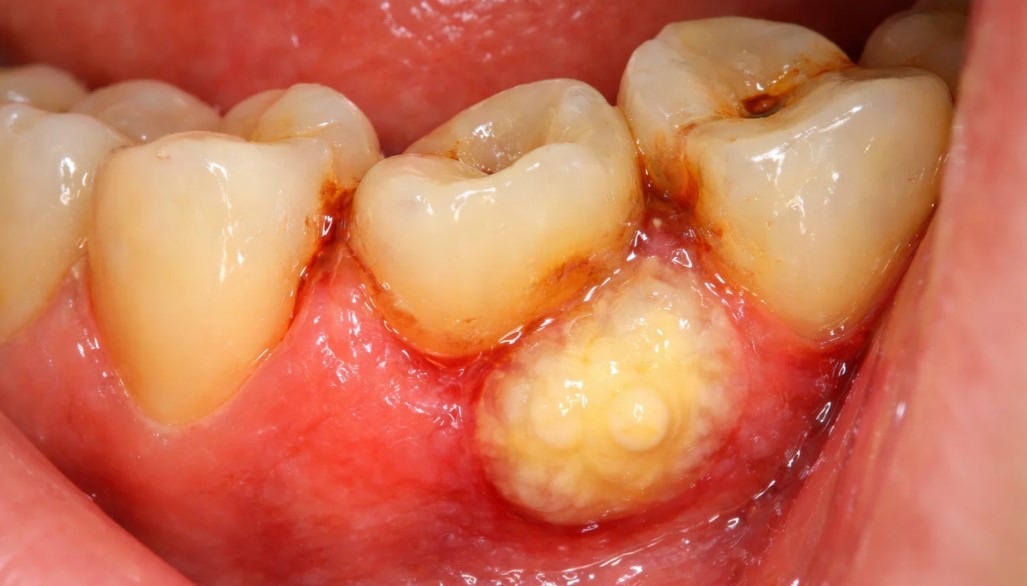
What Is a Dental Abscess?
A dental abscess is a pocket of pus caused by a bacterial infection. It usually forms when bacteria enters the tooth through a cavity, crack, fracture or advanced gum disease.
Common Types of Dental Abscesses
- Periapical abscess: Infection at the tip of a tooth root
- Periodontal abscess: Infection in the gum tissue near a tooth
Dental Abscess Symptoms You Shouldn’t Ignore
Symptoms often worsen quickly and may include:
Most Concerning Warning Signs
- Facial or jaw swelling
- Fever or chills
- Difficulty swallowing or breathing
- Swelling spreading toward the eye or neck
Other Common Symptoms
- Persistent, throbbing tooth pain
- Swollen or tender gums
- Bad taste or foul odor in the mouth
- Pain when chewing
If swelling suddenly drains and pain decreases, the infection is still present—this is not a sign of healing.
When a Tooth Infection Becomes Dangerous
Dentists and physicians consider dental abscesses a medical emergency because the infection can spread beyond the tooth.
Possible Complications
- Jawbone infection
- Infection spreading to nearby teeth
- Sinus infection (especially upper teeth)
- Facial cellulitis
- Bloodstream infection (sepsis)
Adults with diabetes, immune conditions, or heart issues may face even higher risk from untreated oral infections.
Home Remedies vs. Real Treatment
Temporary Relief (Not a Cure)
- Over-the-counter pain relievers (as directed)
- Cold compress on the outside of the face
- Saltwater and baking soda rinses- this is more for periodontal gum infection
What to Avoid
- Applying aspirin directly to the gums
- Using heat on facial swelling
- Waiting to “see if it gets better”
Pain relief does not mean the infection is gone.
How Dentists Treat a Dental Abscess
Treating a dental abscess always focuses on eliminating the infection at its source and preventing it from spreading. The exact approach depends on how advanced the infection is, where it’s located, and the condition of the affected tooth and surrounding tissue.
Below is a closer look at the most common treatment options—and when each one is used.
Draining the Abscess
If an abscess has caused significant swelling or pressure, the first step may be draining the infection.
What this involves:
- A small opening is made to release trapped unwanted infection and bacteria
- Pressure and pain are often relieved quickly
- The area is thoroughly cleaned
Why it’s done:
Drainage helps control the infection and reduce swelling, especially when symptoms are severe. However, draining alone does not cure the abscess—it simply stabilizes the situation so definitive treatment can follow.
Drainage is often combined with a root canal, extraction, or antibiotics, depending on the case.
Root Canal Treatment (Saving the Tooth) & Antibiotics (When Appropriate)
Antibiotics may be prescribed, but they are not a standalone cure for a dental abscess.
Important to know:
Antibiotics help control bacterial spread, but they do not remove the source of infection inside the tooth or gum. Without dental treatment, the abscess always returns.
This is why dentists emphasize that antibiotics support treatment—they don’t replace it.
When the tooth structure is still healthy enough, a root canal is often the preferred solution. The first step is starting a round of antibiotics before root canal treatment, this is because the infection is very acidic and will neutralize the PH of the tissue- making anesthetic less effective. If we start to get the infection under control, we can then assure comfortability during treatment.
What happens during a root canal:
- We make a small access opening on the biting surface of the tooth (that will later be filled at the end of the procedure) and the dying/dead nerves inside the tooth are removed
- The canals are disinfected thoroughly and sealed with gutta percha, a thermoplastic material.
- A crown is usually placed to protect the tooth due to no longer having any blood flow or vitality, the tooth becomes more brittle. The crown gives the tooth more stability, and longevity.
Why dentists recommend it:
A root canal removes the infection while allowing you to keep your natural tooth. For many adults, this is the best long-term option because it preserves chewing function and prevents shifting of nearby teeth.
Root canal treatment is especially common for periapical abscesses (infections at the apex).
Tooth Extraction (When the Tooth Can’t Be Saved)
Sometimes, the tooth is too damaged to safely repair. In those cases, tooth extraction may be the safest option.
When extraction is necessary:
- Severe decay or fracture
- Advanced infection affecting surrounding bone
- Repeated infection after prior treatment
What happens next:
Once the tooth is removed and the infection is cleared, your dentist will discuss replacement options—such as a dental implant or bridge—to restore function and prevent future issues.
While extraction may sound intimidating, removing a severely infected tooth can stop the spread of infection and relieve pain quickly.
What Happens During an Emergency Dental Visit?
Knowing what to expect during an emergency dental visit can ease anxiety:
- Exam and digital X-rays to locate the infection
- Immediate pain and pressure relief
- Treatment plan to eliminate the infection
- Follow-up care to prevent recurrence
Early treatment is usually simpler, safer, and less costly.
Common Myths About Dental Abscesses
Myth: “If the swelling drains, it’s healed.”
Fact: Drainage may reduce pain, but the infection remains and can spread.
Myth: “Antibiotics alone will fix it.”
Fact: Without treating the source, the abscess often returns.
When to Call an Emergency Dentist Immediately
Call for urgent care if you experience:
- Facial swelling
- Fever with tooth pain
- Severe pressure sensitivity
- Trouble swallowing or breathing or fever- (this may be an ER visit)
For adults in the Lansing area, acting quickly can prevent serious complications.
Frequently Asked Questions
Can a dental abscess go away on its own?
No. While pain may temporarily lessen, the infection remains and usually worsens without treatment.
Will antibiotics cure a dental abscess?
Antibiotics can help control infection but typically do not eliminate the source. Dental treatment is still required.
How fast can a dental abscess spread?
In some cases, infection can spread within days. Swelling, fever, or worsening pain should be taken seriously.
Is a dental abscess life-threatening?
If untreated, yes. Severe infections can spread to the bloodstream or airway.
Don’t Wait on a Tooth Infection
If you notice swelling, or severe tooth pain, contact an emergency dentist right away. Early care can protect your health, reduce discomfort, and limit the need for more invasive treatment.
If you’re in or near Lansing and experiencing signs of a dental abscess, call our office immediately at 517-371-5342 for a same-day emergency evaluation.

